HBOT or Hyperbaric Oxygen Therapy refers to operating air pressure above normal atmospheric pressure. It is a unique method of treatment for deep-rooted ailments. The major focus areas of the therapy include serious infections, blood disorders, radiation injury, and diabetes. HBOT is a fast-growing wellness practice in wellness resort business as consumers look for innovative ways to anti-aging and enhancing longevity.
A wound either heals by itself or with some medical interventions. This is what we all expect. But what about those wounds that take a too long time to heal raising the risk of complications? For example, as in diabetics wound healing is a real problem upping the chances of gangrene and amputation.
Lack of oxygen slows down the recovery of wounds. Hyperbaric Oxygen Therapy (HBOT) is considered a more effective treatment where increased exposure to oxygen can quicken the healing. Hyperbaric oxygen therapy is perfect for those who do not like taking pills and other medications to gain weight and reduce stress, depression, and other related problems. It is a safe, inexpensive, spiritual, and non-invasive method of healing.
This wellness guide will detail everything about Hyperbaric Oxygen Therapy:
A Complete Guide to Hyperbaric Oxygen Therapy by Dr. Prem – Introduction, Benefits, Side-effects, Future growth and Much More
-
The Principle
-
Confusing study reports regarding HBOT
-
The science behind Hyperbaric Oxygen Therapy
-
Procedure of Hyperbaric Oxygen Therapy
-
Items Prohibited in HBOT Chamber
-
How much will Hyperbaric Treatment Cost
-
Benefits of Hyperbaric Oxygen Therapy
-
Ailments that can be treated effectively with HBOT
-
Necessary Preparation Before HBOT
-
Precautions Post HBOT Session
-
Risks & Side-Effects Involved
-
What You Should Know Before Undergoing the Therapy
-
Future growth of HBOT
-
Important Factors About Hyperbaric Oxygen Treatment
The principle
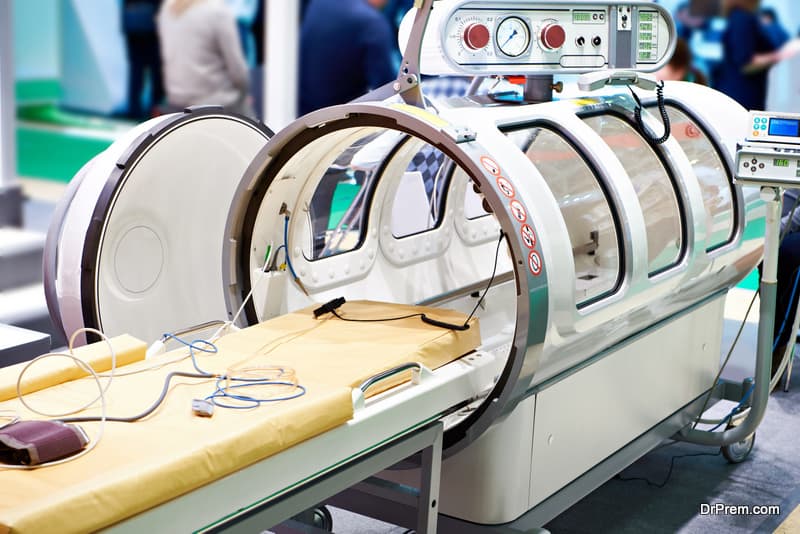
As a biological principle to function efficiently, our body tissues need an adequate and continuous supply of oxygen. When the tissues are damaged, the oxygen requirement increases many times. As HBOT pumps in a larger volume of oxygen in the bloodstream, the normal levels of blood gases are temporarily revived. Tissue function improves as a consequence speeding up the healing process.
Confusing study reports regarding HBOT
The effectiveness of Hyperbaric Oxygen Therapy in healing wounds was discovered accidentally in the 1960s. Later, scientists dug deeper to understand how and to what extent the therapy works.
A 2008 research report from the scientists of Kings College Physician Assistant Program that was released in the Internet Journal of Academic Physician Assistants studied the HBOT benefits in non-healing wounds of diabetics. The results showed HBOT did not have any significant impact or long-term benefits but can be used as a means to postpone amputation.
In 2012, a study report presented in the Journal of Anesthesiology Clinical Pharmacology proved just the opposite. The study conducted by the Postgraduate Institute of Medical Education and Research with a small number of participants found that compared to conventional care in chronic non-healing wounds resulted in a 26% reduction of the wound area, with HBOT it was a 59% reduction.
In a real-life application, a clinical setting of HBOT in the Wound Care & Hyperbaric Center in Lansing, Michigan was in the spotlight in a state journal in 2015. The center applies HBOT for almost every type of wound ranging from arterial ulcers, non-healing diabetic wounds, and postoperative complications to venous insufficiency ulcers. The outcomes are highly satisfactory as revealed by the growing patient footfalls.
The National Center for Biotechnology Information (NCBI) in an article confirms the successful application of HBOT as an adjunct treatment in the healing of wounds.
The science behind Hyperbaric Oxygen Therapy
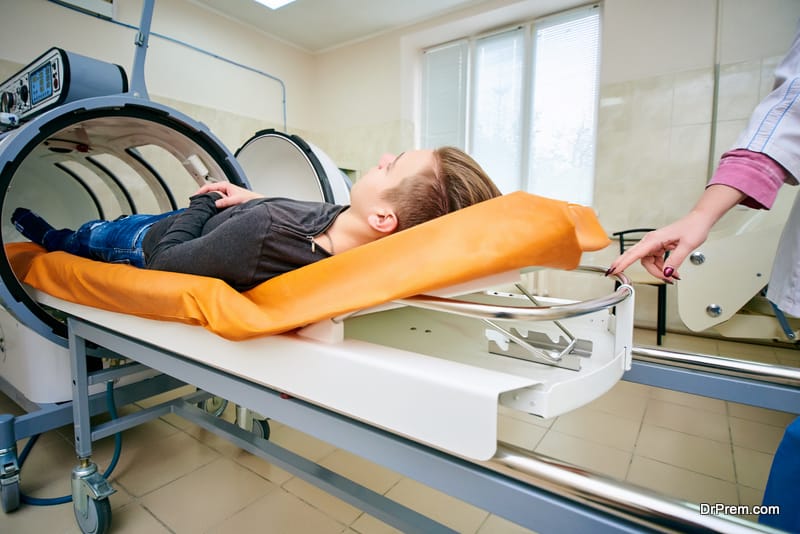
The air that we breathe contains 21% oxygen. In the Hyperbaric chamber, the patients are exposed to 100% compressed oxygen in a chamber. Pure oxygen gets saturated in the blood increasing the oxygen supply to the tissues resulting in fast healing of the wound.
The procedure is technically sophisticated. It enhances the atmospheric pressure equivalent to that experienced at 33 feet below sea level in a 100 % oxygen-rich environment. As the patient breathes in oxygen, it gears up the body’s natural curative process.
The pure oxygen is then transported by blood throughout the body reaching every organ. More oxygen flows into the bloodstream promoting an effective healing process. This extra dose of oxygen supply heals damaged tissues, catalyzes tissue function, and combats infections.
Procedure of Hyperbaric Oxygen Therapy
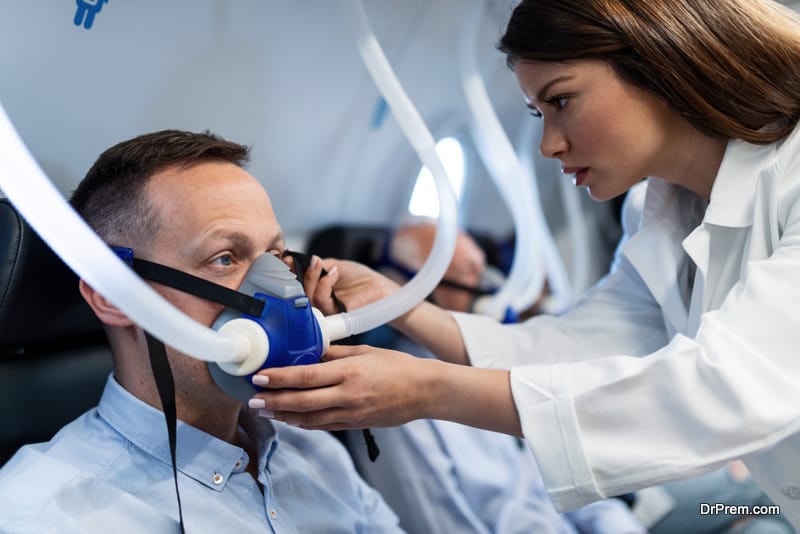
During the therapy session, the pressure of oxygen is raised to three times higher than the normal air pressure present in the air. Skilled, experienced, and qualified practitioners perform the therapy in a specially designed room or chamber known as Hyperbaric Chamber.
Patients are introduced into a specially designed chamber known as the Multiplace chamber or Monoplace chamber. The former allows multiple patients to be treated at the same time while in the later only one patient can be treated at a time.
Most of the reputed clinical settings have monoplace hyperbaric chambers installed. The following steps are involved in a typical HBOT session:
- The patient wearing a 100% cotton gown is asked to lie on a table that will slide into a monoplace chamber. The chamber is a transparent plastic tube 7 ft long.
- The patient is asked to relax and breathe normally when the therapy is on. One can watch TV and listen to music as well. The patient can converse with the therapist and the therapist also keeps a watch on the patient.
- The chamber is then sealed and filled with pressurized oxygen which is 2.5 times higher than the normal pressure.
- The patient may experience mild discomfort in the ears which are quite normal.
- The duration of the therapy may vary from 30 min to 2 hours.
- After the scheduled period, the pressure will be reduced in the chamber and the patient will be taken out.
Items Prohibited in HBOT Chamber
- Electronics
- Watches
- Contact Lenses
- Perfume, Oils, Lotions
- Lighter
- Jewellery
- Hair spray and other hair products
- Nail polish/ Acrylic Nails
- Body piercings
How Much Will the Hyperbaric Treatment Cost

Hyperbaric Oxygen Therapy cost anything from 250$ to 450$ per session. However, it can vary depending on the service locations. The price of the HBOT treatment may not be easily given. The price will depend on the condition to be treated, insurance coverage options, and the number of sessions required for every individual.
You will need to discuss your medical condition and other essential factors with your healthcare provider to get the exact Hyperbaric chamber price for your treatment.
Benefits of Hyperbaric Oxygen Therapy
Although scuba divers and diabetic patients with wounds are usually the initial beneficial focus of HBOT, there are various other patients who can benefit from Hyperbaric Oxygen Therapy. Practitioners believe that this therapy has several other important benefitsthat are mentioned below:
Boosts immunity
Hyperbaric oxygen therapy benefits in boosting the immunity of an individual. It helps to increase the number of white blood cells and white blood cells known as the soldiers of the body because they fight against the harmful bacteria.
Helps in weight loss

Obesity is the key reason for problems like high blood pressure, high cholesterol, and other problems. Hyperbaric therapy helps you to reduce a few inches in very less time. It is not painful and expensive like other surgical treatments as it is an inexpensive and non-invasive method of reducing fat.
Helps in healing
Oxygen is very important to performing internal healing and hyperbaric oxygen therapy helps to increase the flow of oxygenated blood. This helps to heal the body from the inside and promote wellbeing.
Psychological benefits

Many people suffer from problems like stress, depression, and emotional misbalance. The main cause of these problems is energy blockage inside the body and hyperbaric oxygen therapy helps to release the energy blockages.
Helps in the growth of the brain
Oxygen is very important for the growth of the brain as a lack of oxygen in the brain can cause problems like stress, depression, migraine, and anxiety. This unique method helps to increase the flow of oxygenated blood to the brain and helps to reduce these problems.
Ailments that can be treated effectively with HBOT:
- Severe anemia
- Decompression sickness
- Brain abscess
- Sudden deafness
- Skin and bone infection
- Crushing injury
- Diabetic foot ulcer
- Radiation injury
- Skin graft andAlzheimer’s disease
- Vision impairment
- Carbon monoxide poisoning
Just consider what a miracle can an increased supply of pure oxygen under pressure to your bloodstream achieve in terms of curing apparently incurable ailments. Hats off to HBOT and the efforts of medical professionals well acquainted with its application philosophy.
Necessary Preparation Before HBOT
Ear Health Matters
Unsuitable ear health refers to any condition that needs to be cured before undergoing Hyperbaric Oxygen Therapy. If you have flu, ear infection, sinus, cold, or any other ear-related problems talk to your doctor before proceeding with the therapy.
Submit Your Medical History

Patients must submit a detailed history of their previous and existing medical history before going into the oxygen chamber. People with lung diseases are not advised to go for Hyperbaric Oxygen Therapy.
Avoid Smoking and Alcohol

Smoking or the use of tobacco products must be avoided during the HBOT treatment period. These products can counter the benefits of this therapy. The use of alcohol should also be avoided for at least a few weeks before HBOT to avoid complications.
Avoid Perfumes and Other Flammable Substances

Do not apply perfumes, nail polish, deodorant, and other inflammable substances while going for Hyperbaric therapy. The high level of oxygen rises the chances of catching flames, which is why these products should be avoided.
Check Your Medications

Certain medications can interact with Hyperbaric therapy. Inform your health care provider about all the medicines you use. Medicines used for chemotherapies, topic ointments, etc are not advised to be used concurrently with this treatment.
Health Condition is Important

You should consider postponing the therapy if you feel unwell. Wait till you recover. Sickness or health problems such as high blood pressure, fever, flu, loose motions, etc may make it difficult for you to stay in the chamber for the required hours and also delay the effects of the therapy.
Be Careful About Food Consumption

After you consume food, the blood in your body is used in digestion. You should consume food at least an hour or two prior to the HBOT treatment. As the oxygen travels through your tissues and blood vessels, your body should be able to focus on the process.
Precautions Post HBOT Treatment

Risks or side effects post HBOT treatment are mild and last for a temporary period. Some people may experience headache, fatigue, or ear popping; while some may not experience any side effects at all.
However, taking certain precautions may help to avoid the chances of these side effects, such as:
Stay Hydrated & Eat Healthily

You may feel hungry or tired after the HBOT session. It is advised to consume healthy and nutritious food after the therapy. Do not forget to drink a good amount of water throughout the day, your body will require water to avoid dehydration and process the required benefits properly.
Observation and Check-up
Your therapist or the staff will check your blood pressure, pulses, and also your ears immediately post the HBOT session. Blood glucose is also checked for those who have diabetes. Once your team is assured that you are fine, you can leave the center.
Be Easy on Yourself

Although, there are no major side effects of Hyperbaric Treatment that might disturb your daily normal routines; however, your body is explored to experiencing high atmospheric pressure that can impact your body to feel exhausted. Don’t indulge in heavy physical activities, listen to your body and act accordingly.
Risks & Side-Effects Involved
HBOT is normally considered a safe procedure with rare chances of complications but since every treatment carries a certain risk factor, one cannot claim that this therapy is absolutely risk-free.
Some of the proven risks of HBOT include oxygen toxicity, hypoglycemia, and associated seizures and vision changes that may last for one and half month’s post-treatment. Since the chamber is filled with oxygen, there are high chances of catching fire.
It would be not out of place to summarize the possible side effects likely to arise from HBOT.They are:
- Developing barotrauma or discomfort in the ear almost like that experienced in flights.
- Patients can develop tension pneumothorax.
- Near sightedness which goes off in a few days.
- Decompression sickness
- Some patients with congestive heart failure reported additional heart problems after going through Hyperbaric Oxygen Therapy.
The side effects are minimal compared to the immense benefits of the treatment. However, some patients may experience temporary drowsiness and hyperactivity, pain, and discomfort in the ear and sinus due to the change in air pressure. Mild headache and nausea may accompany but are very short-lived.
Note- Not all patients respond equally to all treatments. Often, healing depends on the nature and extent of the wound.
What You Should Know Before Undergoing the Therapy
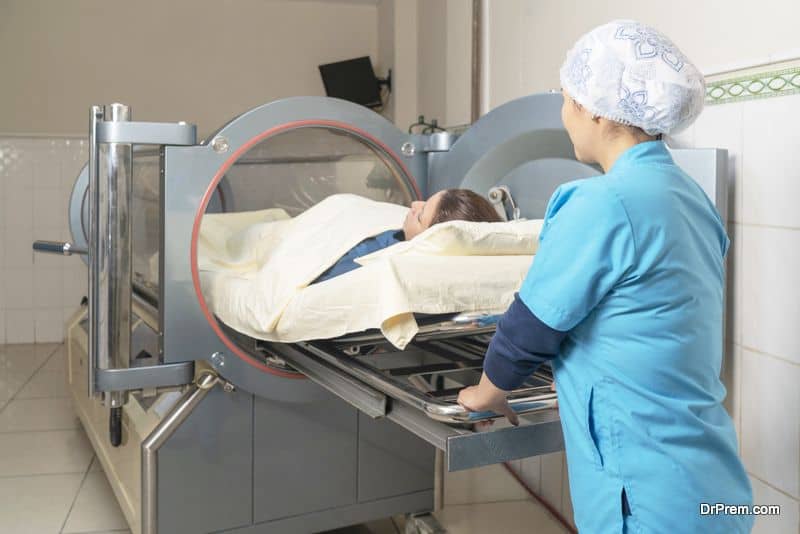
Remember, to avoid HBOT complications, you must take the treatment from professionally trained and certified medical staff only. Some health care providers may or may not be certified in this field. However, Hyperbaric Oxygen Therapy is only performed and supervised by doctors who are specialized in Undersea and Hyperbaric Medicines.
These doctors have proficient knowledge and are well-skilled in treating chronic and acute oxygen-deprived diseases. The procedure is performed by specially trained nurses, technicians, and respiratory therapists under the supervision of these doctors. Ensure these factors before you go for the HBOT Treatment.
This treatment is also provided in various wellness spas and resorts. Hyperbaric oxygen therapy in the wellness resort business is performed by trained and professional staff under the supervision of a certified doctor. It is advised to ensure the authorization of the center before you undergo the therapy.
Future growth of HBOT:
The wide global acceptance of this novel kind of therapy has seen a positive bearing on the sale of equipment related to HBOT. According to a marketing exercise and survey did by Future Market Insights (FMI), the global market for HBOT-related equipment has a promising future with a flourishing Compound Annual Growth Rate (CAGR) of 7.2 % during the projection period.
Acute and chronic wounds inflicting people are expected to rise further in the future. Consequently, the application of HBOT instruments for taking care of the patient’s plight would also shoot up simultaneously.
Important Factors About Hyperbaric Oxygen Treatment
- Hyperbaric Oxygen Therapy is an FDA-approved medical treatment. The oxygen molecules tend to dissolve when delivered at high pressures that help to push the oxygen deep into your tissues, lymph fluids, cerebrospinal fluid, blood plasma, and blood cells.
- The treatment that was unbelievable and laughed at, is today performed over 30,000 sessions per day at the authorized centers across the country.
- The very first Hyperbaric chamber dates back to 300 years ago. It was created by British Physician Hank Henshaw in 1662, who named this chamber ‘Domicilium’. However, this chamber worked with ambient air that was hand-pumped into an airtight vessel with the use of organ bellows.
- HBOT chambers are of two types – Monoplace Chamber and Multiplace Chamber. The monoplane chamber is designed for only one person at a time; the multiplace chamber has a capacity of 18 people at a time. Both chambers offer the same benefits.
- Home hyperbaric chambers are pretty commonly known as the best-kept secrets of Hollywood celebrities. These chambers are in use for the last two decades. After our King of Pop Michal Jackson, Keanu Reeves, and other celebrities are also said to have prescribed home-chamber for their insomnia, young skin, and overall good health.
Summary
Hyperbaric Oxygen Therapy is a unique method of treating various ailments like depression, obesity, joint pains, anxiety, multiple sclerosis, and other treatments. It is generally popular with people who do not like operations and pills, as it is a non-invasive method of treatment.







