Neurology, Brain and Spine
Neurology
In Indian clinics, neurological cases are treated with world class expertise. The patients are offered personalized and specialized healthcare packages to deal with a number of neurological disorders like stroke, head and spinal injuries, brain tumors,ovement issues, seizure disorders, headaches, etc.
Brain and Spine Surgery
Surgery of Spinal Cord Tumors
Surgery for acute head injury and spinal injuries
Treatment includes surgery and reconstruction and done in cases of skull fracture, linear, depressed and basillar skull fractures, minor, blunt and severe head injuries and traumatic conditions.
Micro-Neurosurgery
Surgery for stroke and stroke precautions
Diagnosis ranges from neurological tests, brain imaging tests, blood tests for clotting, electro and echocardiogram. Apart from surgery medication is also recommended by giving blood thinner drugs to the patient.
Laminectomy
Laminectomy is a surgery performed to treat back pain by removing a lamina or bone spur of the spinal vertebrae. This reduces the compression or pressure on the spinal nerve root. The most common laminectomy performed to relieve lower back pain is called Lumbar Laminectomy.
Why is it needed?
Laminectomy is recommended for people who suffer nerve root compression symptoms like:
- Severe leg pain
- Numbness, tingling, and weakness of the legs or buttocks
- Aggravation of pain and symptoms while standing or walking
- Poor bowel and bladder control
- Symptoms not relieved by medication or other conservative treatments and affecting the routine daily life of the patients
Advantages
- Laminectomy improves the quality of life by relieving back pain and increasing mobility.
- One can regain lost control of bowel and bladder.

Disadvantages
- Long recovery time.
- Chances of developing ‘Failed Back Syndrome’ with the possibility of additional surgeries
Causes of nerve root compression:
- Spinal stenosis
- Herniated disk
- Cauda equine syndrome(CES) – loss of bowel and bladder control
- Osteoarthritis
- Tumour
Pre-operative preparation:
- Complete physical examination
- Blood and urinalysis
- Consult with the surgeon week prior and get the correct medicinal prescriptions.
- Inform the surgeon about smoking and alcohol habits.
- Plan for leave from work and domestic help at home.
- Don’t consume anything after midnight before surgery.
- Medical tourists are advised to wear comfortable clothes and select a handicap-accessible hotel room for recovery after getting discharged from the hospital.
Facts and figures
- The 4th and 5th lumbar vertebrae discs are the most common site for operation for almost 95% of surgeries.
- An ancient Egyptian surgeon spoke about lumbar vertebral disorders in literature in 3000B.C
- Dr. Victor Alexander Haden Horsley, professor of surgery at University College London, performed the first laminectomy in 1887.
- Back pain is more common in men than women, and in adults between 45-64 years.
- 1 in5 people are vulnerable to back pain, the leading cause of maximum missed workdays, and 13 million people visit healthcare providers for the same reason every year.
Risk and Complications
- Reaction to anesthesia or medication
- Infection or pain
- Blood clots
- Damage of the spinal nerve leading to paralysis later on
Precautions
- Take medicines and perform exercises as prescribed by the surgeon and physiotherapist respectively.
- Keep the incision area dry and clean
- Avoid strenuous activities and twisting at the hips and shoulders for 6-8 months
- Use arms to support the body while getting out of bed
- Avoid waist banding
- Lie on the back with a pillow under neck and knee
Spinal fusion
Why is it needed?
Done mostly at the lumbar vertebrae, the surgery is advised to treat the back pain or neurological deficit which has not responded to conservative treatment. This includes
-
- Degenerative disk disease
- Spondylolisthesis
- Spinal stenosis
- Scoliosis
- Fracture
- Infection
- Tumour
Advantages
- Brain tumor removal surgery which is successful, saves and extends patient life
- Spinal lumbar fusion increases the stability of the spine that reduces the chances of injury to the lumbar spine.
- In cases of severely injured spinal vertebrae, spinal fusion decreases the chances of further injury and promotes healing.

Disadvantages
- Premature and inappropriate fusion procedures or a ‘Failed Back Surgery’ will bring you back to square
Facts and figures
- First Russell Hibbs and Fred Albee developed the concept and methods for bony fusion of the spine to treat the Pott disease in 1911
- According to published data, more than 400,000 spine fusion surgeries, the most serious age-related change, are performed in the United States annually
- The spectacular increase in the number of fusion surgery had been observed in the past two decades in the American population
Preoperative Preparation
- Complete physical examination
- Blood and urinalysis
- ECG and chest X-ray
- Consult with the surgeon week prior and get the correct medicinal prescriptions.
- Inform the surgeon about smoking and alcohol habits.
- Plan for leave from work and domestic help at home.
- Medical tourists are advised to wear comfortable clothes and to select a handicap-accessible hotel room for recovery after getting a discharge from the hospital
Post operative care
- Most patients are required to stay at the hospital on medications for 4-6 days and fed through IV for 2-3 days after the operation.
- The spine needs to be kept in the right position to maintain alignment for a few days. The drainage tube will be removed within 2-3 days post-surgery.
- In physiotherapy, the patient will be trained on how to sit, stand, and walk wearing a back brace to ensure proper healing.

Precautions
- Take medicines and Perform exercises as prescribed by the surgeon and physiotherapist respectively.
- Keep the incision area dry and clean.
- Avoid strenuous activities for at least 6-8 months
Brain Tumor Surgery
Brain tumor surgery is done to remove brain tumour, primary or secondary. In most cases, brain tumor is removed via the craniotomy procedure. In craniotomy, a lesion/tumor in the brain is removed by making an opening in the cranium (skull).
Why is it needed?
Symptoms
- Headache, which gets worse on waking up, but reduces in a couple of hours
- Headache which gets worse with exercise and coughing
- Headache even during sleep
- Headache associated with double vision, confusion and vomiting
- Weakness in one part of the body
- Seizures
- Altered mental functions
Other associated symptoms may include
- Changes in smell, taste, alertness, sensation-hearing
- Motor function loss- bladder and bowel, balance, coordination, swallowing
- Eye abnormalities-uncontrollable movements, different pupil size
- Tremors in hands, difficulty in writing
- Obesity
- Symptoms due to pituitary tumor
- Symptoms related to hormonal imbalance
- Sensitivity to cold and heat
- Low blood pressure
The causes for primary brain tumor are unknown. The risk factors for brain tumor development are:
- Exposure to radiation at work , head injuries
- Radiation therapy to brain
- Hereditary
Facts and figures
- Usually, brain tumour are found to be more common in men than in women
- Early diagnosis as well as excellent treatment helps to cure many non-malignant tumors and some malignant tumors. Long term rate of survival for non-malignant tumors is 95%, and some kinds of malignant tumors is 80%
- In US, every year, 1,500 children and 21,000 adults are diagnosed with benign and malignant tumors in the US
- Brain tumor occurs mainly in people aged over 65. However, brain tumors are second most cancer in children, especially children below 8 years
Risk and Complications
- Brain tissue injury
- Blood vessels injury
- Nerve damage causing weakness or muscle paralysis
- Reaction to medication or anesthesia
- Return of tumor growth
- Seizures
- Coma
- Bleeding
- Strokes
- Swelling of the brainPossible Complications
- Infection in the brain structures
Advantages
- Brain tumor removal surgery which is successful, saves and extends patient life
- Patients get relief from symptoms and can continue to live with improved quality of life
- A surgeon named William, was the first surgeon to remove brain tumor in 1879
Disadvantages
- Sometimes, surgery on a particular part/area of the bone can cause the loss of some mental functions such as – speech related disorders, memory, muscle weakness, imbalance, coordination, vision and so on. These disorders can last for a short or long duration, and sometimes, never go away
- Chance to develop fatal brain herniation
Preoperative Preparation
- Complete physical examination
- Blood and urinalysis
- Diagnostic tests like X-Rays, arteriogram, MRI, CT scan
- Consult doctor about the risks, post surgery rehabilitation as well as the possible outcome of surgery.
- Consult doctor week before surgery to get list of medicines to be stopped and taken
- Inform the surgeon about alcohol or smoking habits
- Arrange for a caregiver post surgery (for home, driving and rehabilitation program)
- Arrange blood donation/donors as blood may be required during surgery
- Medical tourist should book a hotel room suited for patients who have undergone surgery
No eating or drinking after midnight before the surgery
- Wear loose fitting comfortable clothes
- Patient head has to be shaved before surgery
Post operative care
- Usually, a patient has to stay at the hospital approx 7-14 days after the surgery. Patient is shifted to ICU immediately after surgery, where vital signs are constantly monitored. Once the patient stabilizes, he/she is shifted to a normal room and his brain functions are monitored closely by doctor and staff. Medication is given to control any pain and avoid infections
- The incision is covered with bandages, which has to be removed and replaced regularly
- Patient is allowed only intravenous fluids for the first few days
- Physical therapy is started during the hospital stay, to help patient improve strength, speech, daily living skills. Normally, patients experience emotional changes and feel discouraged and tired after surgery. The positive attitude and cheerful manner of friends and family is required to help the patient overcome emotional trauma
Dos, Don’ts and Precautions
- Do keep the scalp clean and dry, till sutures are removed
- Do take enough rest
- Don’t lift heavy weights or perform strenuous activity
- Do follow the post surgery care instruction prescribed by surgeon meticulously
- Do monitor changes in speech, mental ability, and keep doctor updated about these
Full recovery usually takes 8 weeks to 2 months after surgery. Surgery outcome depends on the site and type of brain tumor, type of surgical procedure and the general health of the patient.
Bell’s Palsy Treatment


Why is it needed?
This condition can recover with or without treatment. However, medical treatment enhances recovery and helps with the following:
- Eye protection
- Prevent infections
- Reduced inflammation
- Fast recovery
Advantages
- Reduces swelling of the facial nerve
- Prevents eye scratches or poking
- Improves muscle movements
Disadvantages
- Side-effects of medications
- Weight gain
- Agitation
Facts and figures
- Surgery is not usually performed to cure this condition. Proper treatment can help in quick recovery.
- There is no root cause yet found for this condition.
- People with Lyme disease, diabetes, HIV/AIDS, sarcoidosis, pregnancy, cold virus, flu, or middle ear infections are at high risk.
- Bell’s Palsy treatments are often focused on the eye, as affected people can find it difficult or impossible to close their eyes.
Symptoms
- Sudden weakness on one side of the face
- Difficulty closing lips and eye on the affected part
- Stiffness and drooling from the affected side of the mouth
- Drastic change in facial expression
- Hypersensitivity to sound
- Facial pain
- Drooping eyebrow
- Experiencing usual sensations on the face
Risks & complications
- Surgical risks
- Permanent hearing loss
- Injury to the facial nerve
Rare risks of Medications
- Weakness, weight gain
- Feet Swelling
- Behavior change
Post-Treatment Care
- Physiotherapy and massages should be done diligently
- Regularly brush and floss your teeth to avoid tooth decay or dryness
- • Use prescribed medications only to heal the facial nerve problem
Precautions
- To help right diagnosis inform the doctor if you had any major changes or stress.
- Wear eyeglasses or goggles to prevent dirt and dust from entering your eyes.
- Avoid chewy, hard, stringy food with skins, shells, and husks (lettuce, raw tomatoes, chewy meats, peas, etc.)
- In case of any facial pain, inform your doctor for medication.
- Keep cloth soaked in warm water on the affected side 4-5 times a day to get relief from facial pain.
Blood Clot Brain Surgery
Why is it needed?
- Restore blood flow to vital body organs
- Fight life-threatening complications
- Reduce the risk of severe disabilities
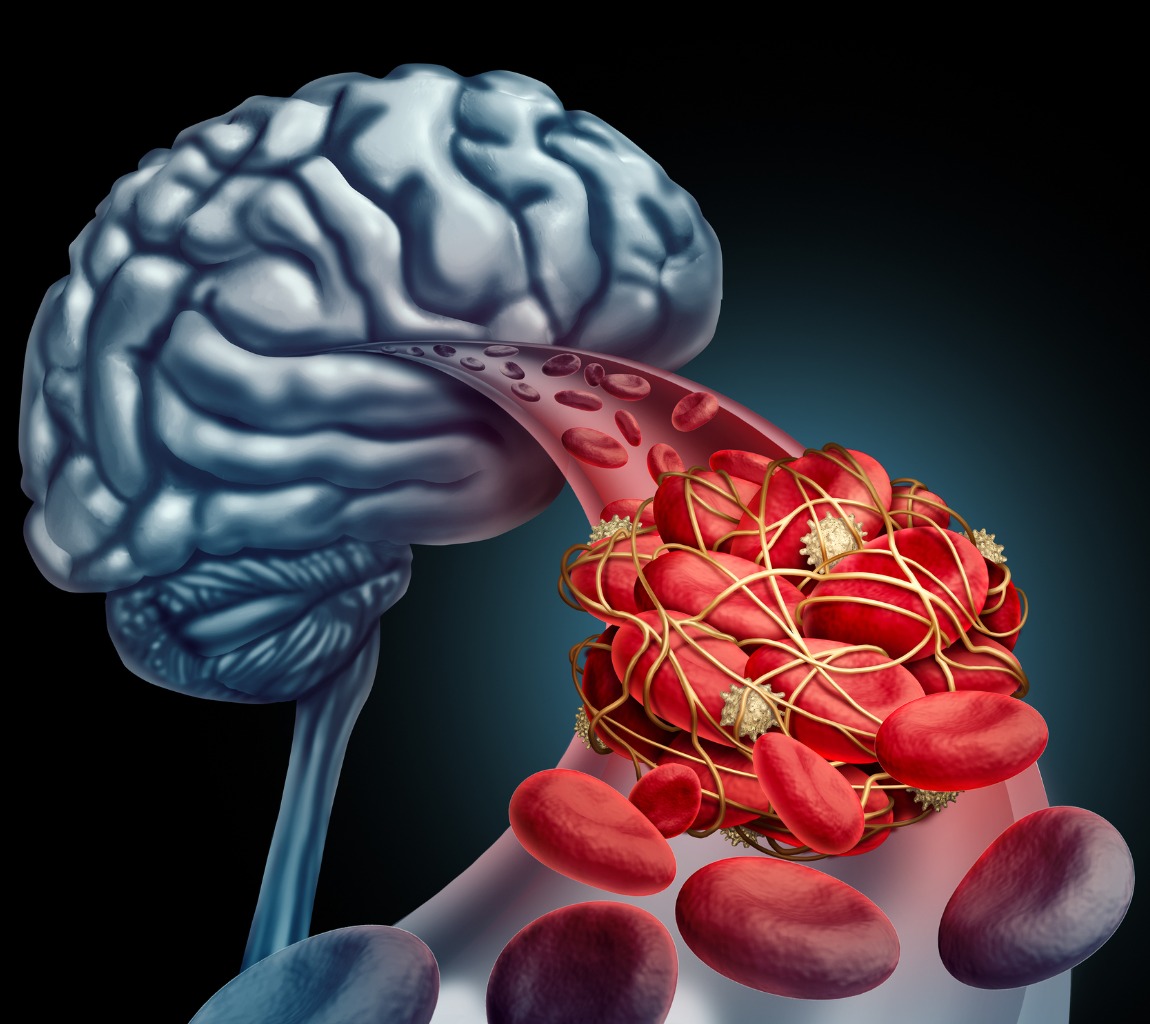
Advantages
- Prevent Stroke
- Improved Recovery
- Opportunity for an independent life
Disadvantages
- Various restrictions till recovery
- Wound or infections
- Temporary problem with speech, muscle weakness, etc
Facts and figures
- As said by Neurologist Irene Katzan, innumerable evidence has proven that stress is a high-risk factor for causing blood clots leading to ischemic strokes.
- A surgical method ‘Stent retriever technology’ approved by FDA in 2015 plucks a blood clot in the brain with a tiny wire trap, providing quicker recovery and long-term results.
- With the use of prescribed injections and medications, doctors often try to dissolve the clot to restore blood flow without surgery.
Symptoms
- Severe headaches
- Loss of consciousness
- Inability or unclear speech
- Weak or changed vision
- Confusion
- Disorientation
- Difficulty in using limbs and walking
Pre-operative care
- Several imaging such as MRIs, CT-Scans, and ultrasounds are required to help surgeons with detailed images of the size and location of the clot to plan the surgery.
- If the patient has smoking habits, it is a must to discuss a smoking cessation plan before the treatment. As it can cause complications during and after the surgery.
- Make sure to list any vitamins, over-the-counter drugs, or herbal supplements the patient uses to prevent its interactive reactions.
Risks & complications
- Bleeding
- Infections
- Hematomas
- Damage to blood vessels or stenosis
- Pulmonary embolism
- Reoccurrence of the clot
Precautions
- The patient will be discharged after 3 to 7 days post-surgery. However, proper care must be taken at home for at least 12 weeks at home till the recovery.
- Use of any other medications or supplements except the prescribed ones must be cross-checked with the doctor before use.
- Activities such as strenuous exercises, chores, driving, and lifting heavy objects are restricted for weeks post-surgery.
- Educate and learn about the after-effects of the treatment to keep yourself mentally prepared and recover better.
Cerebral Angioplasty
Why is it needed?
- Narrowed or blocked coronary arteries
- Restricted blood flow to the brain
- Abnormal or damaged blood vessels
Advantages
- Identifies and examines abnormalities
- Gives a detailed and clear picture of blood vessels
- Minimizes complications before surgery
Disadvantages
- Transient ischemic attack
- Pain and discomfort
- Potential allergic reaction
Facts
- This is a popular surgery to remove the plaque that blocks arteries or blood vessels.
- Cerebral angioplasty does not require stitches. Apparently, only some pressure is used for stopping the bleeding and the operated site is covered with a dressing.
Symptoms
- Loss of balance
- Extreme dizziness
- Troubled speech and understanding
- Sudden weakness in one side of limbs or face
- Severe headaches that occur suddenly
- Vision disturbance in both eyes
Pre-operative care
- Diagnostic tests and physical evaluation are performed
- Current medications or treatment details, allergies, and medical history should be informed
- Blood thinning medications and diabetic drugs are usually stopped before the procedure
- Use of any substances or smoking is strictly advised to be stopped
Risks and Complications
- Damage to the blood vessels
- Puncture to artery
- Formation of blood clots
- Infections
- Bleeding
- Stroke
- Kidney failure
- In-stent restenosis
Precautions
- A patient might experience swelling and bruising after the procedure. If you notice any signs of coldness/pain/redness in limbs, signs of drainage, etc. inform the doctor.
- If the patient experiences a fever over 100 degrees Fahrenheit take medical help.
- Do not ignore any serious side effects or discomfort.
- Follow proper safety measures prescribed by your doctor to avoid complications.
Cranioplasty
Why is it needed?
- Skull vault defect
- Severe trauma to the head
- Syndrome of the trephined
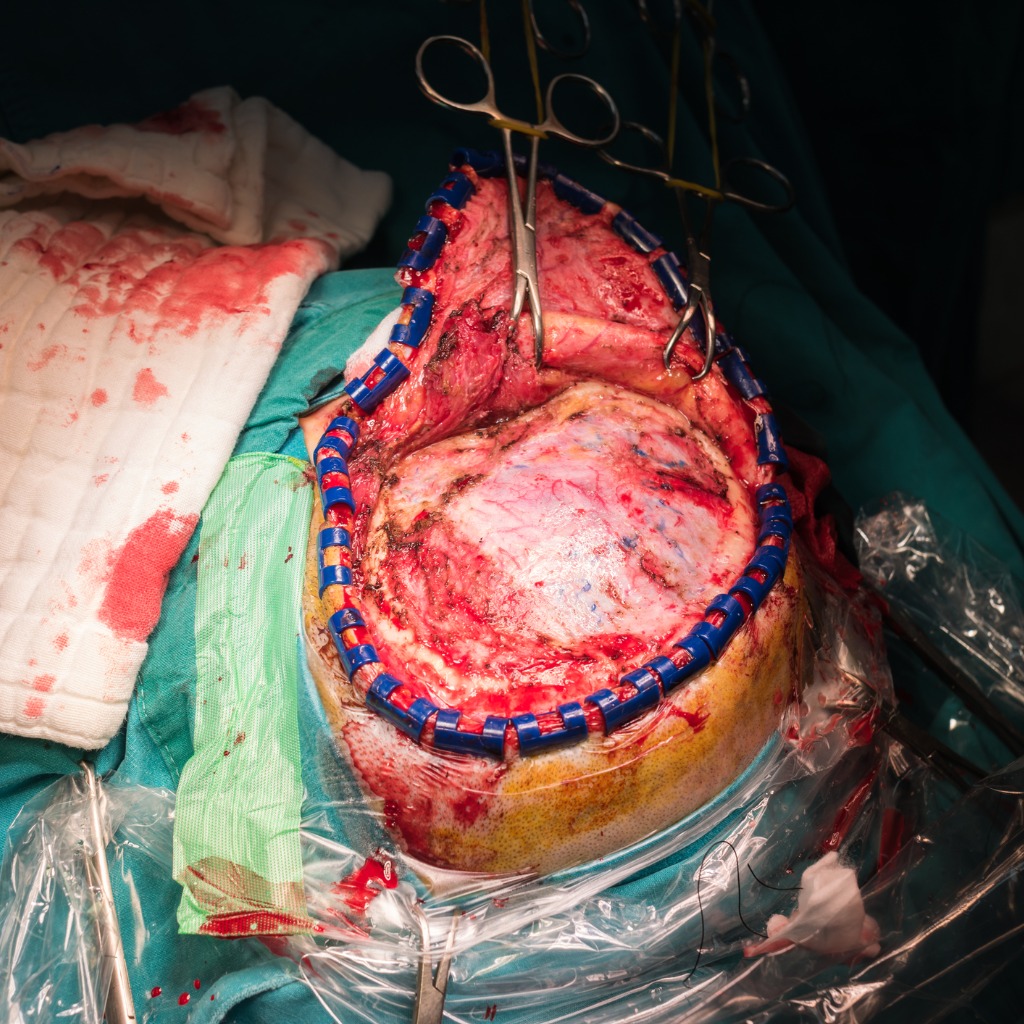
Advantages
- Improves neurological function
- Provides brain protection
- Restores damage after secondary causes
Disadvantages
- Intermitted headaches
- Potential infections
- Swelling
Symptoms
- Increasing headaches
- Depressed Fractures
Facts and figures
- Cranioplasty is prepared before the surgery takes place. This method is known as Prefabricated implants with 3D design and printing. leading to excellent results from the procedure.
- The surgery may seem like very painful. However, the pain mostly involves typical headaches that are managed with injections and pain relief medicines prescribed by your doctor.
Pre-operative care
- Inform your doctor if you have any health problems, especially blood clotting conditions
- Provide your medical history along with all required tests to your surgeon
- Use of any substances like tobacco, alcohol, smoking, etc must be stopped 1-2 weeks before surgery
- Patients should not consume any food items at least 8 to 12 hours before the procedure
Risks and Complications
- Stroke
- Seizures
- Formation of blood clots
- Urinary infection
- Pneumonia
- Bone resorption
Precautions
- The patient will be on activity restriction post-surgery. Activities such as driving, weight-lifting, exercises, etc must be avoided for at least 8 to 12 weeks.
- The surgery can be used to treat different conditions. Ask your doctors about safety measures to be followed particularly.
- Keep away from chronic stress.
Craniotomy
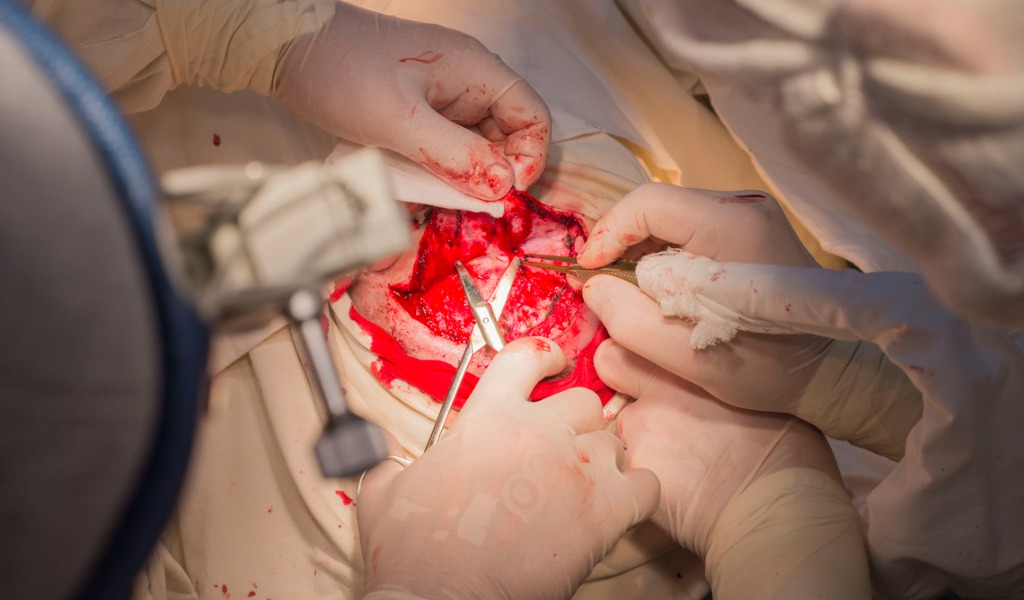
Why is it needed?
Neurological surgeons decide the procedure required to treat patients under craniotomy surgery who suffers from:
- Brain cancers
- Brain infected with different bacteria, especially with the genus meningococcus
- Increased blood pressure in the brain due to internal bleeding
- Cerebral Edema
- Formation of abscesses within the brain
Advantages
- Helps in diagnosing and treating brain tumors
- Treats Parkinson’s and epilepsy.
- Repairs brain tissues
- Removes blood clots and blood leakage
Disadvantages
- Nerve damage
- Swelling of the brain
- Loss of certain mental functions
Symptoms
- Blurred or doubled vision
- Weakness in arms, face, or leg along with difficulty in walking
- Eythrima, leaking fluid, swelling, or increased warmth of the skull
- Involuntary twitching of limbs
- Experiencing stiffness in the neck
- Fits or seizures
- Redness, swelling, or pain in legs or forelimbs
- Difficulty in remembering things
Facts and figures
- A part of the skull flap (covering of the brain) is removed to access the brain and is replaced after the surgery is done.
- Computerized guidance system is usually used to perform Craniotomy surgery.
- The word Craniotomy is derived from the Latin word ‘cranium’ meaning ‘skull’ and the Greek word ‘tomy’ meaning ‘cutting’. It literally refers to the opening of the skull.
- There is a type of craniotomy surgery, known as ‘awake craniotomy’ or ‘awake brain surgery’, which is performed while the patient is still awake.
Pre-operative care
- Do not consume any food or liquid before the surgery
- Certain tests are performed for checking neurological problems
- Inform your doctor about all your medications and herbal supplements
- Submission of medical history is required
- Area around the operating site should be shaved
- Allergies, especially to anesthesia or latex must be informed
- The patient will receive a tranquilizer before surgery
Risks and Complications
- Pneumonia
- Unsteady blood pressure
- Seizures
- Weakness in muscles
- Chances of infections
- Cerebrospinal fluid outflow
- Bleeding
Precautions
- Do not smoke, until the complete recovery post-surgery
- Diligently follow the recovery plans and follow-ups after surgery
- Do not use unprescribed painkillers without informing your doctor
- If you experience chest pains, fever, fatigue, seizures, swelling, or troubled breathing, talk to your doctor immediately.
Spinal Stabilization
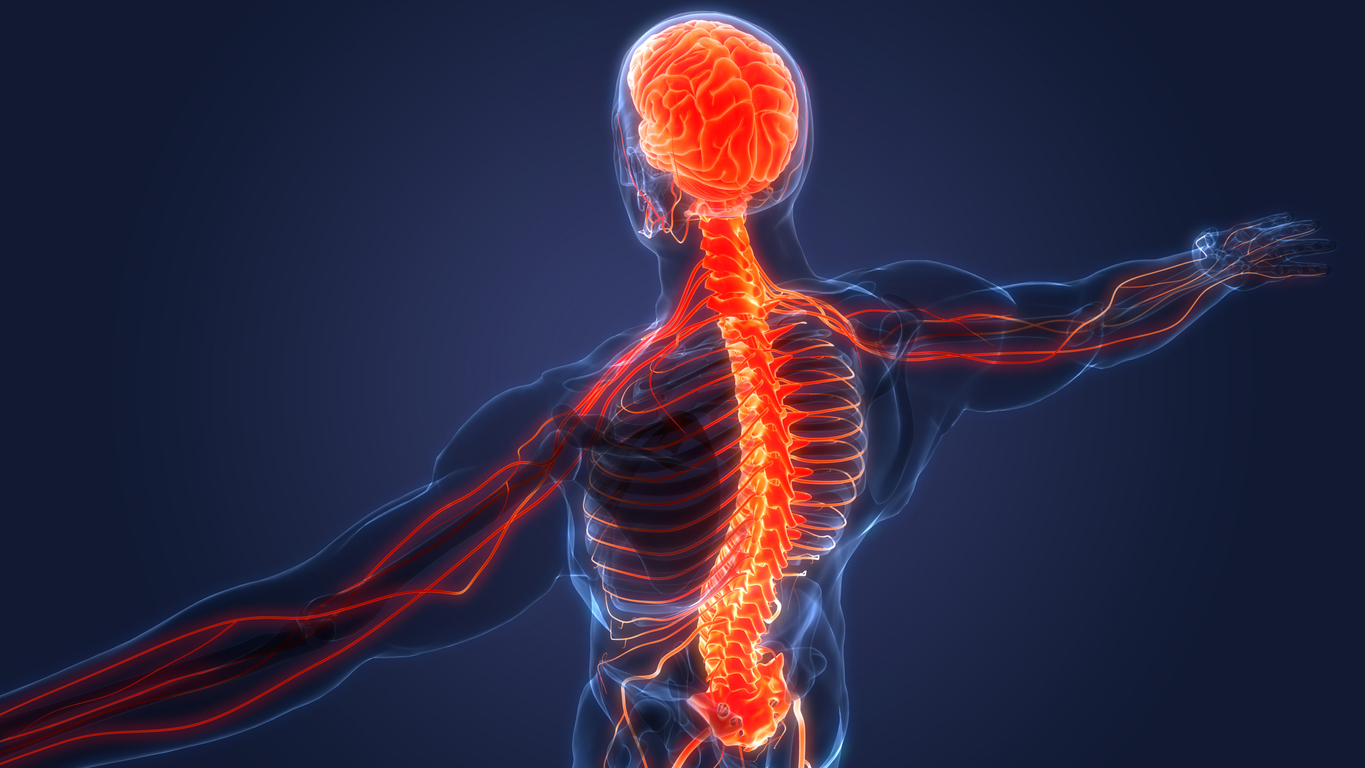
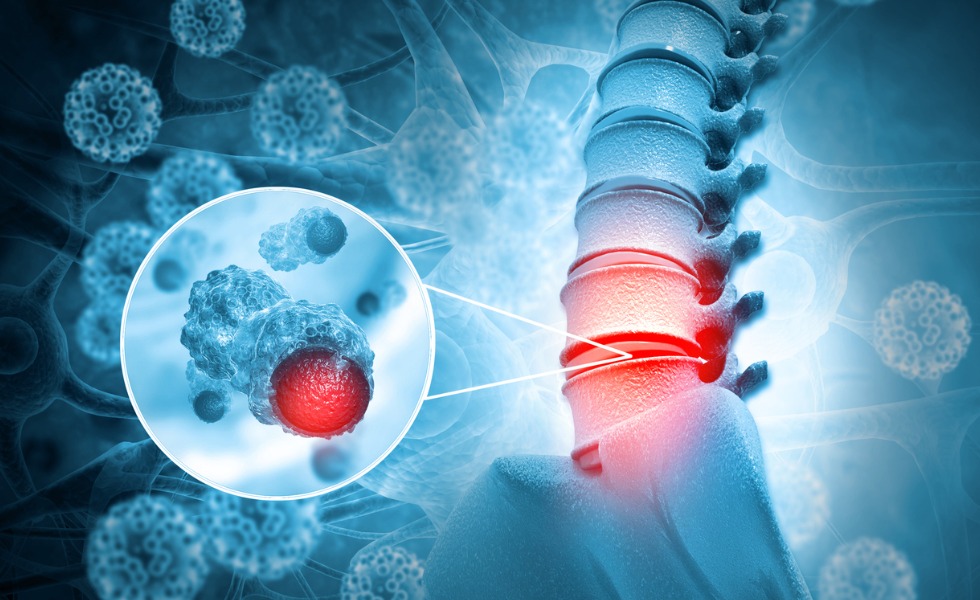
Why is it needed?
Normally, physicians try different methods before opting for this surgery. Some conditions that require this solution are:
- Spinal compression
- Osteoporosis
- Spinal tumors
- Blunt force trauma
- Weak or unstable vertebral column
- Hernia in the disc
Advantages
- Reduces back and neck pain
- Improves spine stability and support
- Strengthens muscles in the spine
Disadvantages
- Fever accompanied by chills
- Bleeding or blood clots
- Infections
Risks and Complications
- Poor wound healing
- Damage to nerves and blood vessels
- Dural tear
- Persistent pain
- Graft site pain
Facts and figures
- Spinal stabilization also helps with facet arthropathy, chronic back aches, and spondylolisthesis.
- Bone graft is used during the procedure of spine stabilization surgery. The material can either be used from your own body (pelvis) or taken from bone banks.
- Tradition method of spine surgery involved a large incision to operate the spine, cutting of tissues and muscles, and a long recovery time.
Symptoms
- Failure in leg or arm movements
- Unnatural positioning of the head
- Rigidity or pressure in the neck
- Lack of control in bladder or bowels movements
- Back pain
- Headaches
- Unconsciousness
- Prominent locomotion problems
Pre-operative Care
- Medical history, use of alcohol or smoke, and allergies are checked
- Several spine imaging are required before surgery
- Any type of jewelry, dentures, contact lenses, and piercing must be removed
- It may be required to take antibiotics, to monitor unhealthy bacterial growth.
- The area of the operating site should be properly shaved.
- Any problems in the blood pressure or pulses are tested.
Precautions
- Use of braces is necessary if prescribed to help the spine alignment correct
- Physiotherapy must be done regularly to heal and maintain spine orientation
- Bed rest for at least 3 days is required after the surgery
- Lifting heavy objects or performing strenuous activities is highly not recommended
- Experiencing some pain is normal, however, only prescribed pain relief medications should be used.
- Bending, lifting, and twisting must be avoided.
Kyphoplasty


Why is it needed?
- Strengthen bones
- Nullify microbial flora effects
- Correct inflammation of the vertebra
- Regain normal structure of the spine
Advantages
- 70% to 80% pain reduction
- Significantly improved mobility
- Improved quality of life
Disadvantages
- Pulmonary embolism
- Leakage of bone cement
- Intense allergies
Causes
- Metastatic tumors
- Osteoporosis
- Bone Marrow infections
- Cancer-damaged vertebra
- Increasing back, neck, or head pain
- Spinal Fracture
Facts and figures
- The first Kyphoplasty was done in 1998 by an orthopedic specialist Mark Reiley, with successful results.
- The surgery involves minimal incisions and has a success rate of 96% with rare complication possibilities.
- Kyphoplasty surgery also helps to increase the height of the patient by repairing spine fractures and overall structure.
- A small balloon is inserted in the problematic place and then is inflated to give a temporary stable structure before the specialized cement filling is used.
Rare Risks
- Amplified back pain
- Allergic reactions to cement filing, chemicals, or dyes used during x-rays
- Bleeding
- Weakness or numbness due to damaged nerves
- Addition compression fractures
- Paralysis
Pre-operative Care
- Pulses and blood pressure will be tested a day before surgery
- Hypersensitivity and allergies toward any medicines should be informed
- Several imaging such as X-ray, CT-Scan, or MRI of the vertebra are performed
- Localized or total anesthesia is applied, depending on the state of the patient
- No food is allowed at least 6 hours before surgery, and two hours for water
Precautions
- Various minerals, vitamins, or medical drugs are prescribed to strengthen the vertebra
- Physical activities are restricted by the surgeons for some time after the surgery
- Movements such as bending, stretching, lifting, and twisting, must be avoided till recovery
- Back brace must be worn while walking or sitting for proper support, only except for sleeping.
- Do not drive at least for 2 weeks post-surgery
Microdiscectomy
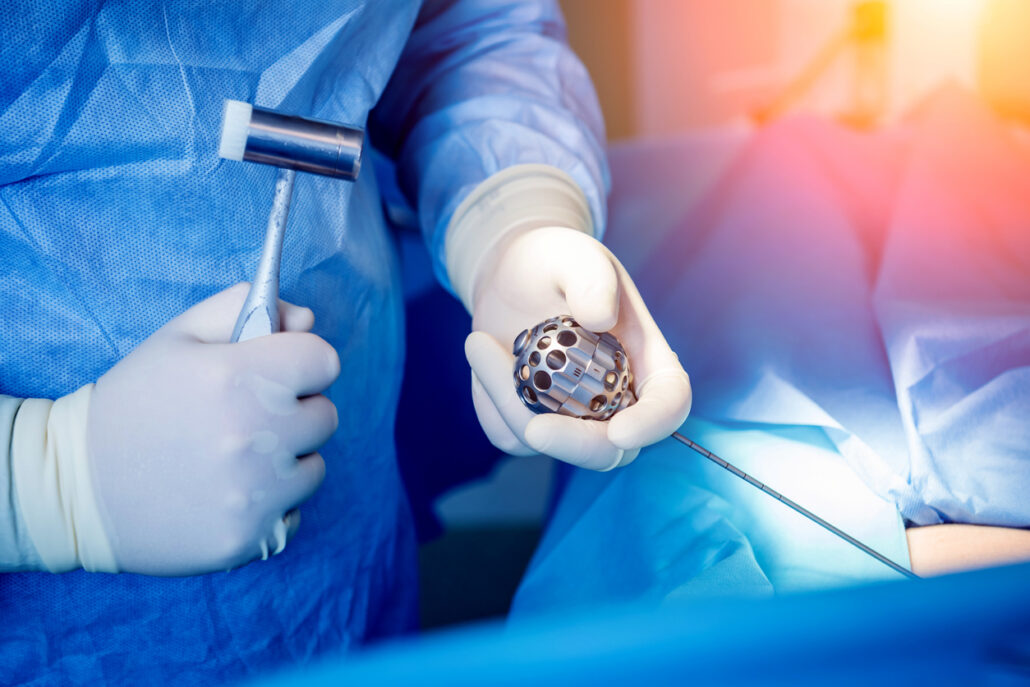
Why is it needed?
Microdiscectomy is usually used by the neurologist to cure the anomaly caused due to vertebral disk ruptures such as:
- A small portion of the intervertebral disc is broken out of the spinal vertebra resulting in extreme pressure on the spinal cord or nerves.
- Another condition is where the disc is in intact structure but is grown symmetrically causing force on spinal nerves or vertebral neurons.
- Both of the above-mentioned conditions lead to serious injury to the nerves in the spine causing pain.
Advantages
- Abolished or reduced leg pain
- Improved leg and back mobility
- Strengthened spine
Disadvantages
- Deep vein thrombosis
- Spinal cord fluid leakage
- Blood vessels or nerves injury
Causes
- Obesity or overweight
- Back muscle sprain
- Occupational hazard
- Loss of water content in spinal disc
- Genetic predisposition
- Blunt force trauma (rare case)
Facts and figures
- As per 2008 research, 80% to 90% of patients who underwent LMD felt it was worthwhile in curing leg pain caused by disc herniation.
- The procedure of microdiscectomy is minimally invasive. Thereby usually people are discharged to go home within 24 hours.
- The surgery is most effective in the first 6 to 9 months when symptoms start. However, if the nerves are compressed for too long, they may not revert back.
Risks and Complications
- Redness or swelling
- Infections
- Re-herniation of disc
- Dura tear
- Pneumonia
- Post-Surgical Bleeding
- Blood Clots
Pre-operative Care
- Narcotic use, medical history, and allergies are verified
- Detailed imaging of the spinal cord is done
- As per the type of surgery, numbing agents are used
- Required antibiotics and painkillers are given to manage the pain
- Nothing should be consumed after midnight before the surgery
- You must not use any cosmetics, perfumes, lotions, etc. prior to surgery
Precautions
- Braces are necessary to keep the accurate orientation of the backbone
- Follow physiotherapy regularly for better healing and recovery
- You must avoid lifting heavy objects or strenuous activities for 6 to 8 weeks
- Keep your doctor informed about any side effects or if too much pain is noticed
- Make sure to perform all required follow-ups and prescribed exercises
Brachial Plexus Injury
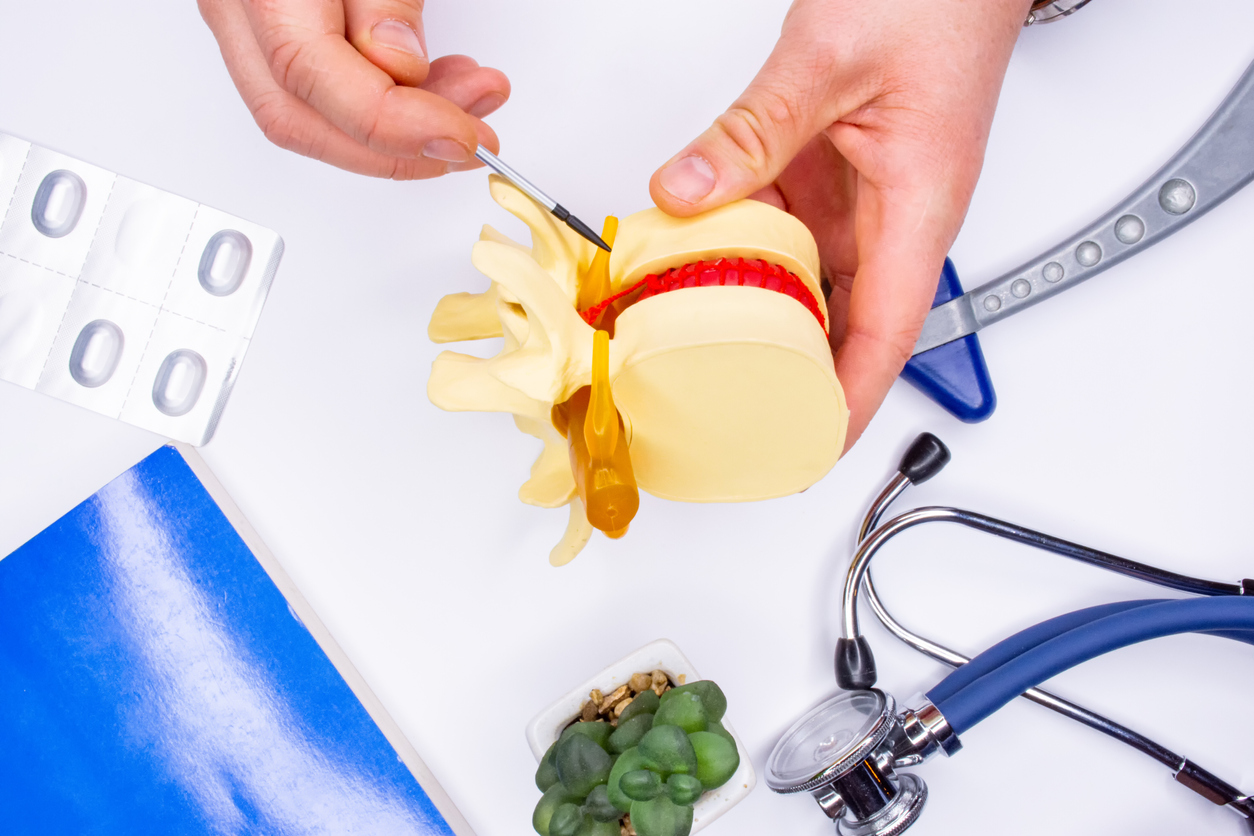
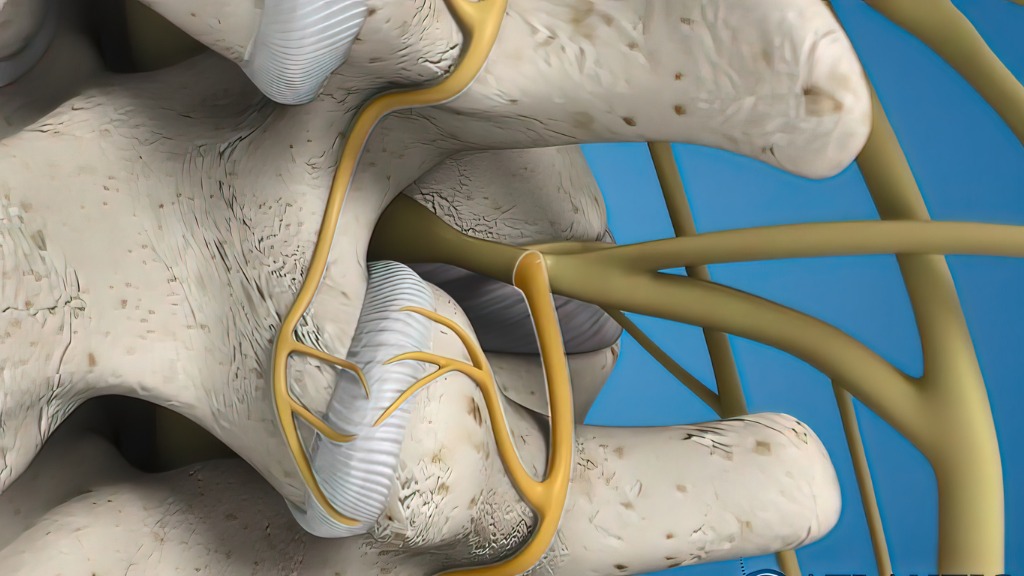
Why is it needed?
The treatment of Brachial plexus can either be surgical or non-surgical. The treatment depends upon the age of the patient, intensity, type of injury, and duration after the injury as per the following:
- Surgical treatment – It is needed when the injured nerves are unable to recover on their own. This leads to disruption in their normal functioning as well.
- Non-Surgical treatment – It is used when the nerves can recover in a few weeks or months with therapeutic movements, different types of therapies, or physical treatment.
Advantages
- Proper working of joints and muscles
- Range of motion is maintained
- Prevents stiff joints
Disadvantages
- Reduced balance and coordination
- Decreased strength
- Joint dysfunction
Risks
- Permanent disability
- Burn injuries and numbness
- Muscle atrophy
Causes/ Symptoms
Minor Injury:
- Numb sensation in the arm
- Feeling of shooting downs in the arms
- Getting burning or shocks sensation
Severe Injury:
- Complete numbness in arms, hands, and shoulder
- Inability to move
- Weakness in moving particular muscles of arm, hands, or shoulder
- Severe pains
Facts and figures
- It is highly recommended to treat brachial plexus injury in 6 months for the best chance of healing and recovery
- The time of Brachial plexus surgery can range anywhere between 3 to 12 hours. It will however depend on the complexity of the case.
- Brachial plexus injury can also occur due to birth trauma, gunshot wounds, cancer, accidents, radiation therapy, and athletics.
- As per the 2020 study, brachial plexus injuries in adults and teens have increased over a decade due to vehicle accidents (Motorcycle accidents 67%, Car crashes 14%).
Pre-operative care
- For an in-depth understanding of the injury, Electro diagnostic studies are performed including SNAP, NCV, SSEP, and EMG
- Advanced imaging studies are done such as CT scans and MRI
- Submission of medical history and complete clinical examination is mandatory
- Follow every precaution suggested by your surgeon to avoid complications
Precautions
- It can take a few months or a year for complete healing, proper motion movement exercises, therapies, and check-ups are a must for faster recovery.
- Use of splint or sling is prescribed, to keep the injured arm in an accurate position after the surgery.
- Physical therapy is essential after brachial plexus surgery. The duration, type, and timing of the therapy are decided as per the type of surgery.
Deep Brain Stimulation
Why is it needed?
Deep brain stimulation surgery is given to those who have issues caused by discrepancies in impulse generation. Some diseases that are treated or some symptoms that can be halted are:
- Epilepsy
- Parkinson’s disease
- Huntington’s disease
- Dystonia
- Tourette syndrome
- Traumatic brain injury
- Multiple sclerosis
- Depression
- Chronic pain
- Dementia
- Addiction
- Tremors
Advantages
- Individualized treatment
- Symptom reduction
- Decreased need for medications
Disadvantages
- Expensive
- Surgical side effects
- Awake and invasive procedure
Risks and Complications
- Inflammation or pain in the grafting area
- Seizures
- Difficulty in thinking
- Confusions
- Stroke
- Infections
Facts and figures
- In 2011, scientist and neurosurgeon Kim Burchiel introduced “asleep” DBS. It works with the help of CT scans and MRIs taken before and during the surgery which enables surgeons to place leads exactly in the right place.
- One may think, that after brain surgery, the patient may require to stay at the hospital longer. Patients usually get discharged in a day or two after the leads are placed.
- Deep Brain Stimulations were originally developed and used as a therapeutic solution to treat people with chronic pain and behavior disorders.
Symptoms
- Damaged muscle strength and flexibility
- Not feeling senses in the body.
- Lost, blurred, or doubled vision
- Problem in synchronization
- Back pain going down to other body parts
- Seizures or shivers
- Difficulty in remembering things
- Incoherent speech
- Reduced cerebral activities
- Impaired understanding and expressions
Pre-operative Care
- Patient’s medical history, use of sedatives, allergies, etc are studied in detail
- Any complication in blood pressure or pulses are tested
- You will be instructed on how to bathe and will be provided special shampoos to prepare your skin before the surgery.
- There should be no food consumption at least 8 hours before surgery
- The operation site will be shaved by the hospital staff only
Precautions
- There might be a mild imbalance for a few weeks after the surgery. It is advised to have a company for support.
- Having residual pains is normal after the surgery. However, only prescribed antibiotics and pain relievers should be used to control it.
- The stimulation can be manually controlled using the remote control given.
- Swimming, use of scrubs, or harmful strong shampoos should be avoided.
- Let your comfort level be your guide, and do not rush to do any strenuous activities.
- Consume a healthy and light diet at least 2 weeks after the surgery, diet can be increased as per individual tolerance.
Brain Tumor Treatment
Why is it needed?
- Mass of tissue formed in tumors can cause extreme pressure on the brain leading to loss of functions and severe pain.
- Tumors tend to have their blood supply and can leach upon the blood supply required in the brain.
- Brain tumor treatment is essential to prevent disruption in neural activities and normal functioning of the brain.
- The treatment of brain tumors comprises chemotherapy, radiotherapy, or surgeries in extreme situations.
Advantages
- Removable of tumor at large volume
- Slows down or shrinks growth
- Kills Cancer cells
Disadvantages
- Several side-effects
- Frequent hospital visits
- Skin and hair problems
Precautions
- Avoid hazards environment
- Exposure to radiation
- Maintain proper hygiene
- Consume a healthy and nutritious diet
- Avoid any toxic and harmful substance use
- Stay away from chronic stress